
The Vagus Nerve & the Parasympathetic Nervous System
The vagus nerve is the main communication pathway between the brain and most internal organs. It is a key component of the parasympathetic nervous system, often described as the body’s “rest and digest” system.
- Heart rate and breathing
- Digestion and gut activity
- Stress recovery and emotional balance
- Immune responses and inflammation
When vagal signaling is reduced or impaired, the body may struggle to shut down inflammation effectively.
Source: Tracey KJ, Nature 2002
Why Cymba Conchae?
Not all ear-based stimulation is the same. The cymba conchae is unique because it is the only area on the skin surface that is consistently and exclusively innervated by the vagus nerve. This makes it the most direct, precise, and scientifically supported access point for non-invasive vagus nerve stimulation (taVNS).
Anatomical studies show that 100% of examined ears contain vagus nerve fibers in the cymba conchae, while other areas—such as the tragus or ear canal—show large individual variation. In contrast, regions like the earlobe contain no vagal innervation at all and are therefore often used as sham controls in clinical studies.
100% of examined ears contain vagus nerve fibers in the cymba conchae.
Source: Peuker ET, Filler TJ. Clin Anat. 2002
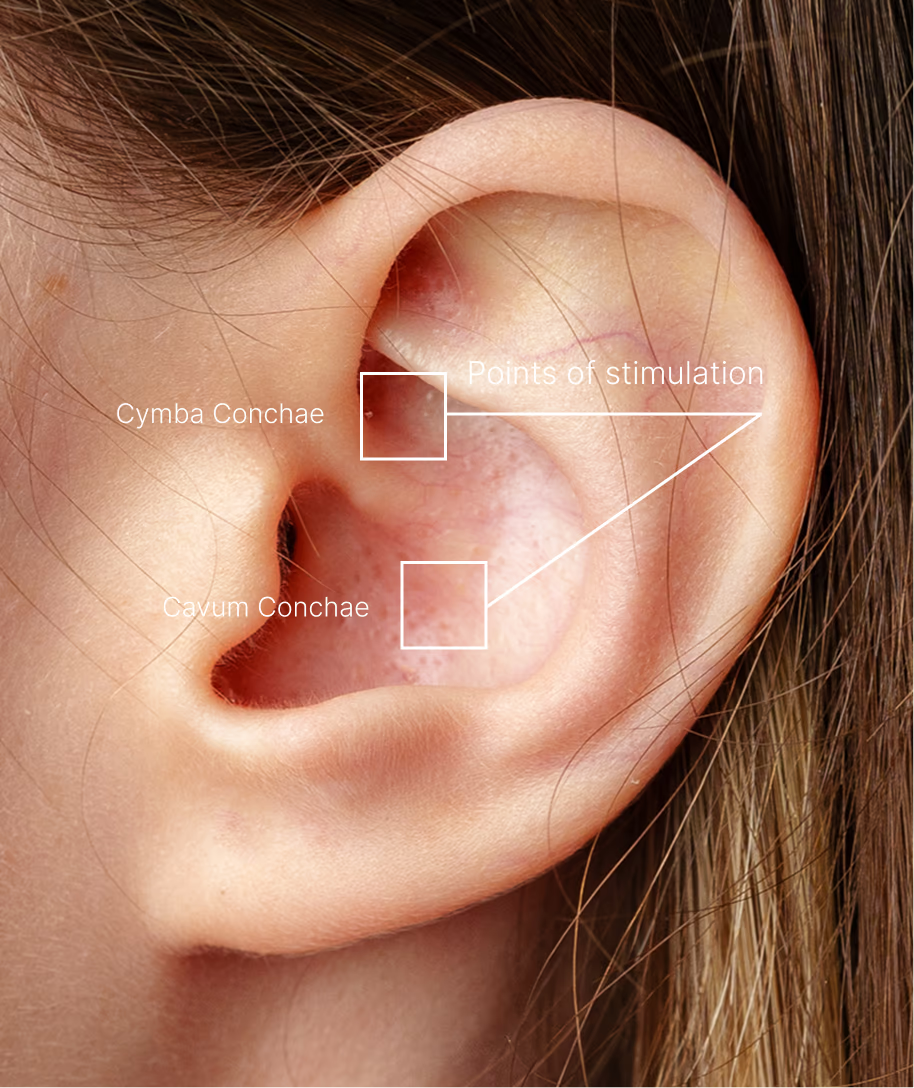
Functional MRI (fMRI) research confirms these findings. Stimulation of the cymba conchae produces the strongest activation of vagal brainstem pathways, including the nucleus tractus solitarius (NTS) and locus coeruleus—key hubs involved in autonomic regulation and the inflammatory reflex. The resulting brain activation pattern closely resembles that seen with invasive cervical vagus nerve stimulation, but without surgery.
This is fundamentally different from external neck, chest, or wrist devices that deliver weak, unfocused currents and primarily stimulate skin, muscle, or blood vessels rather than the vagus nerve itself. In contrast, proper ear-based VNS targets a real vagus nerve entry point, enabling reliable engagement of brain–immune communication. Cymba conchae–based taVNS: location determines biology, and biology determines outcomes.
"Cymba conchae–based taVNS: location determines biology, and biology determines outcomes."
Site
Vagal innervation
Evidence for activating the inflammatory reflex
Cymba conchae
High, consistent
Strongest
Cavum conchae
Moderate
Moderate
Tragus
Variable
Mixed
Lobule
None
Often used as sham
Source: Yakunina N et al. Neuromodulation 2017

What Is Inflammation
Inflammation is a natural and essential response of the immune system. In the short term, it helps the body fight infection and repair tissue damage. This type of inflammation is called acute inflammation and is usually beneficial. Problems arise when inflammation does not shut off. Chronic inflammation is a prolonged, dysregulated immune response that can damage tissues and contribute to pain, fatigue, autoimmune disease, and long-term illness.
For many years, inflammation was thought to be regulated only by immune cells and chemical signals. Research now shows that the nervous system plays a central regulatory role.
Source: Tracey KJ, Nature 2002;
Andersson & Tracey, Annu Rev Immunol 2012
10th cranial nerve
The vagus nerve is the 10th cranial nerve and a central regulator of calm, recovery, and internal balance.
one mainrecovery system
The vagus nerve is the core of the parasympathetic “rest and digest” system that helps the body recover from stress.
200K nerve fibers
Each main vagus nerve (one on the right and on on the left) contains 100,000 fibers, enabling rapid and precise brain–body communication
The Inflammatory Reflex
The inflammatory reflex is a brain-controlled neural circuit that monitors immune activity and actively suppresses excessive inflammation. It works much like other reflexes in the body, such as those that regulate heart rate or breathing. When inflammatory signals rise, sensory fibers of the vagus nerve detect these signals and relay the information to the brainstem and the brain. The brain then sends signals back through the vagus nerve to calm immune activity. This discovery fundamentally changed how inflammation is understood: the immune system is regulated by the brain.
Source: Tracey KJ, Nature 2002
How the Inflammatory Reflex Works
Sensing inflammation
Inflammatory molecules such as cytokines are detected by sensory fibers of the vagus nerve.
Brain integration
These signals are received in the brainstem, primarily in a region called the nucleus tractus solitarius (NTS) and then relayed to multiple brain regions.
Suppressing inflammation
The brain sends signals back through the vagus nerve, triggering the release of acetylcholine. This neurotransmitter binds to specific receptors on immune cells and suppresses the production of inflammatory cytokines such as TNF.
This mechanism allows the body to actively turn down inflammation in real time.
Source: Andersson & Tracey, Annu Rev Immunol 2012
Acute vs. Chronic Inflammation
Acute inflammation is the body’s natural, short-term response to injury or infection. It helps eliminate threats and supports healing, typically resolving once the problem is addressed. Chronic inflammation occurs when this response fails to switch off and this process is generally harmful.
Progress toward symptom improvement
Progress toward symptom improvement
Clinical and pilot studies suggest that improvements from vagus nerve stimulation typically develop gradually over weeks rather than days. Early biological effects may appear within the first week, followed by more substantial symptom improvement with continued use over subsequent weeks.
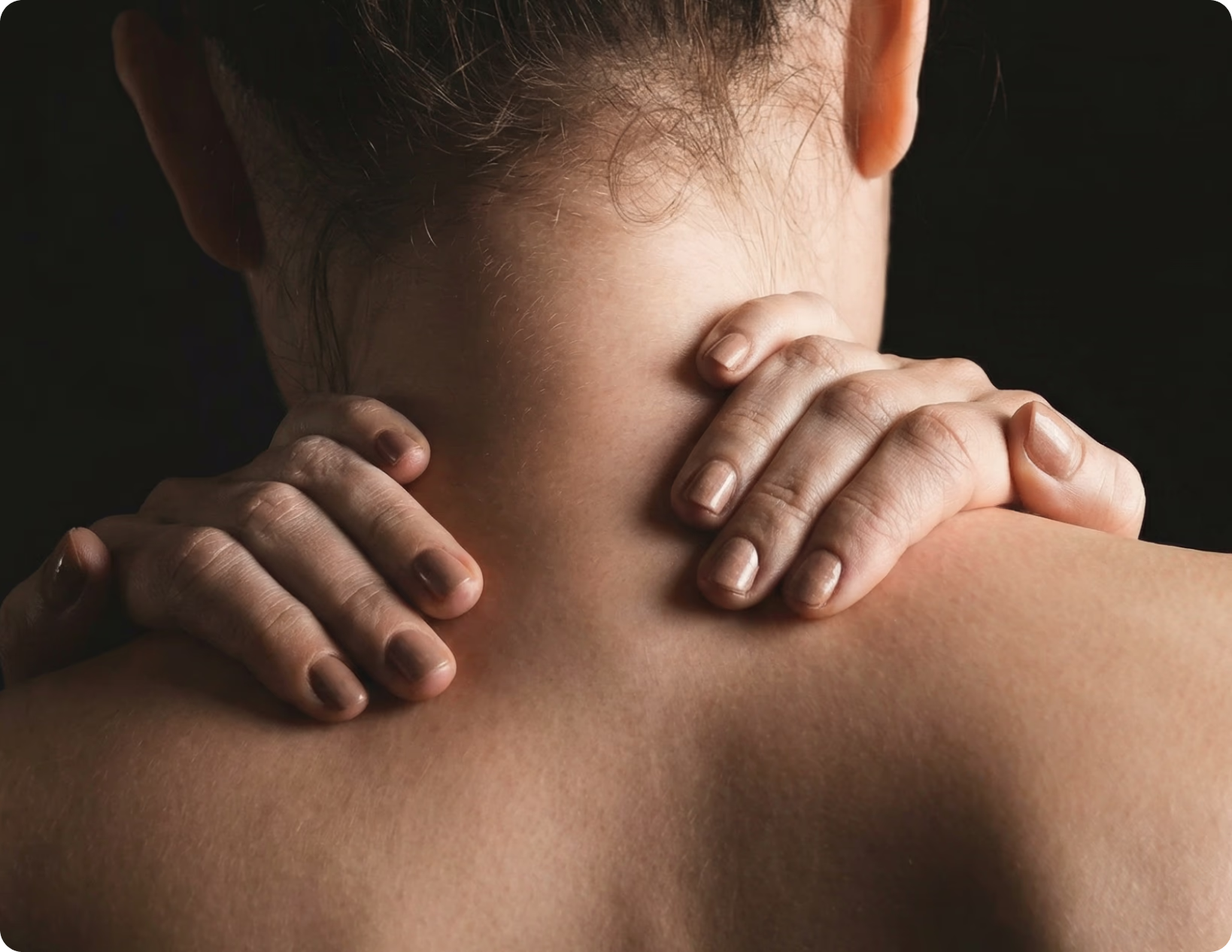
Chronic Inflammation Is a Failure of Biological Control
When inflammation fails to switch off, it becomes a driver of chronic disease, disability, and cost.
From Healthy Regulation to System Failure
Acute Inflammation
- Triggered by injury or infection
- Resolves within hours to days
- Localized to affected area
- Activates healing cascade
- Self-limiting feedback loop
Chronic Inflammation
- Persistent, uncontrolled immune activation
- Inflammation remains continuously active
- Causes pain, fatigue, and functional decline
- Drives long-term disease progression
- System remains dysregulated
Examples of Chronic Inflammatory Conditions
- Cardiovascular diseases
- Long-COVID
- Metabolic syndrome
- Rheumatoid arthritis
- Diabetes
- SLE
- Obesity
- Inflammatory bowel diseases
- Alzheimer
- Psoriasis
- Cognitive decline
- COPD
- Depression
- Osteoarthritis
- Generalized anxiety
- Low back pain
- Multiple sclerosis
HRV, Autonomic Balance & Immune Regulation
Heart rate variability (HRV) is commonly used as a marker of autonomic nervous system activity and overall well- being. Higher HRV is often associated with better stress resilience and recovery.
However, HRV reflects the balance between parasympathetic and sympathetic activity, not the activity of the vagus nerve alone. Importantly, HRV does not directly measure activation of the inflammatory reflex or immune regulation.
For this reason, HRV may be useful in some cases for assessing general wellness and autonomic balance, but it remains unproven whether HRV can be used to predict the vagus activities in immune modulation.
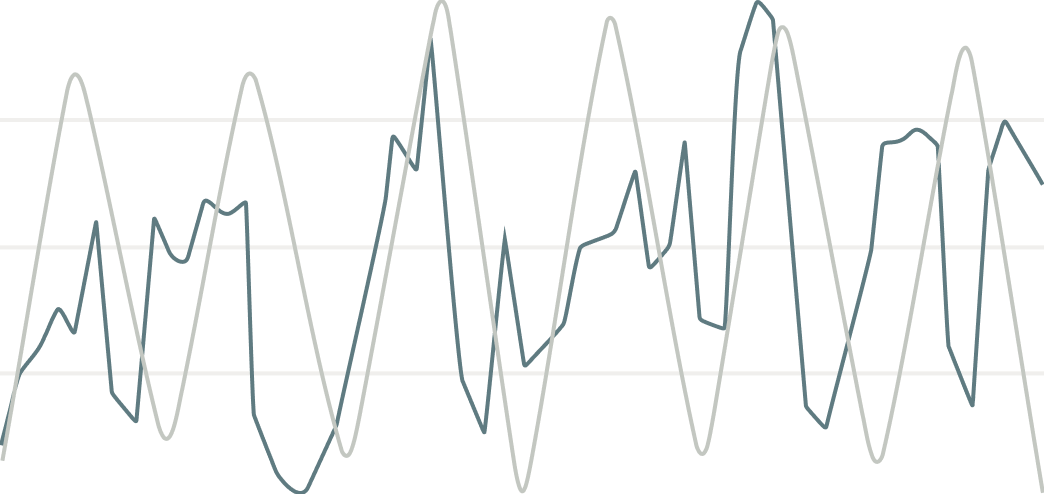
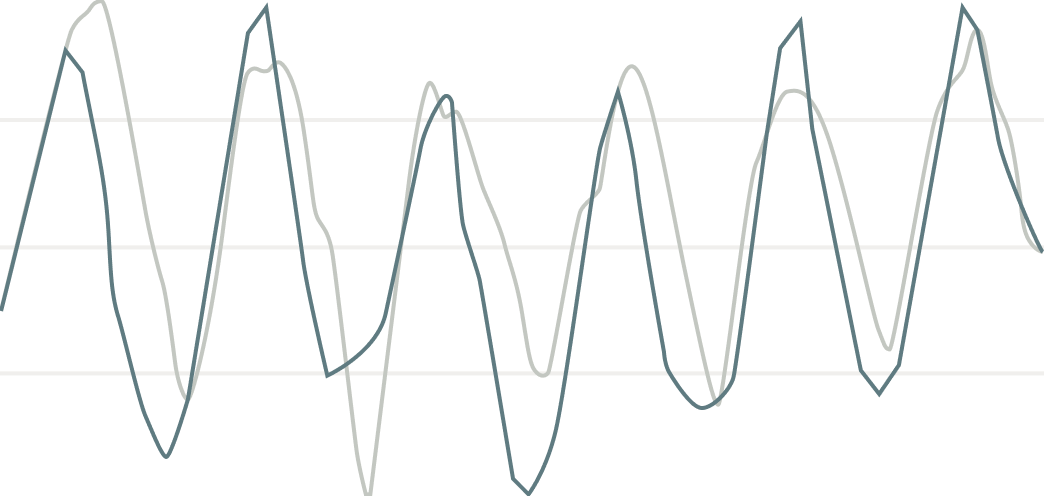
This graph shows that before ear-based vagus nerve stimulation, breathing and heart rate were poorly synchronized, and that full, healthy synchronization was restored 1 hour after stimulation.
